INTERSTITIAL LUNG DISEASE- SYMPTOMS, CAUSES & TREATMENT
Overview
Interstitial lung disease ild disease is a term for a group of disorders that cause inflammation and scarring in the lungs. The scars which are associated with interstitial lung disease affect the ability to breathe and get enough oxygen into your bloodstream. It can be caused by long-term exposure to dangerous substances, such as asbestos. There are a few types of autoimmune diseases, such as rheumatoid arthritis, which can also cause interstitial lung disease. In some cases of ild disease, however, the causes remain unknown.
Moreover, this disease can be caused by medicines, radiation therapy, connective tissue disease, or inhaling pollutants. Lung damage caused by ild disease is not reversible. Medicines can slow the damage of interstitial lung disease, but many people will never be able to fully use their lungs again. Lung transplantation is an option for some people with this disease.
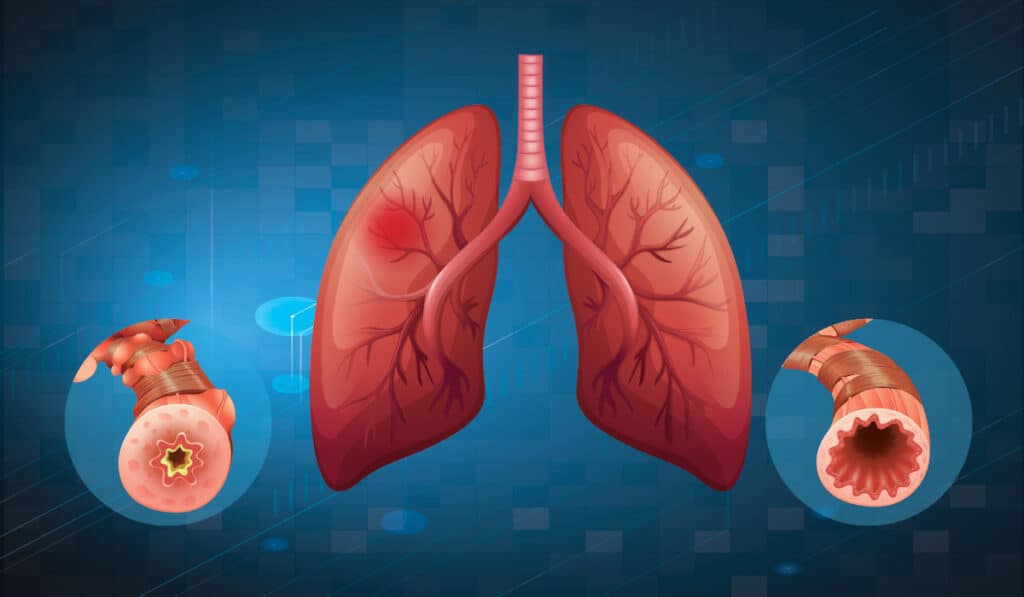
What is Interstitial Lung Disease
ILD or Interstitial lung disease is a term for a group of over 200 disorders that cause inflammation and scarring in your lungs. ILD damages the tissues between the small air sacs called alveoli and the surrounding blood vessels. This makes it harder for you to get oxygen from your lungs to your body. The other term for Interstitial lung disease is diffuse parenchymal lung disease.
What Exactly Happens in ILD?
When you have ild disease, the parts of the lungs that allow oxygen to reach the blood and tissues are damaged. Scars in the lungs make it difficult to breathe and you may have a chronic cough. Tiredness is due to a lack of oxygen. As the damage worsens, you can develop life-threatening complications, such as lung infections and respiratory failure very less oxygen or very high carbon dioxide in your body.
Examples of Interstitial Lung disease
There are more than 200 ild diseases. The most common is idiopathic pulmonary fibrosis, followed by diseases caused by occupational exposure or connective tissue disorders. Some other examples are Asbestosis, Silicosis, radiation pneumonitis., Nonspecific interstitial lung disease.
Risk Factors of Interstitial Lung Disease
You can suffer from ild disease if you are
- Age – ild is mostly seen in adults over 70 years old
- If you have gastroesophageal reflux disease
- If you have a history of Smoking and active smoking can worsen the condition.
- If you have a history of certain diseases or conditions, such as hepatitis C, tuberculosis, pneumonia, COPD, or connective tissue disease.
- If you work on substances that can irritate the lungs, such as asbestos, silica, mold, fungus, or bacteria. This is an occupational or environmental toxin effect.
- If you have chest radiation or chemotherapy.
Causes:
Let us see the Causes of interstitial lung disease
- Occupational and environmental factors
Long-term exposure to a variety of toxins and pollutants can damage the lungs such as
- Silica dust
- Asbestos fibers
- Grain dust
- Bird and Animal poop
- Radiation treatments
- Indoor whirlpools
Some people who receive radiation therapy for lung or breast cancer show signs of lung damage months or sometimes years after initial treatment.
- Medicines
Many drugs can damage the lungs, particularly
- Chemotherapy drugs that are designed to kill cancer cells, such as methotrexate and cyclophosphamide, can also damage lung tissue.
- Medicines for the heart. Some drugs used to treat irregular heartbeats, such as amiodarone (Nexterone, Pacerone) or propranolol (Inderal, Innopran), can damage lung tissue.
- Certain antibiotics like Nitrofurantoin and ethambutol can cause lung damage.
- anti-inflammatory drugs. Some anti-inflammatory drugs, such as rituximab (Rituxan) or sulfasalazine (Azulfidine), can cause lung damage.
- The damage to the lungs can also be the result of car immune diseases such as:
- Rheumatoid arthritis
- Scleroderma
- Dermatomyositis and polymexitis
- Mixed connective tissue disease
- Sjogren syndrome
- Sarcoidosis
The list of substances and disorders that can lead to interstitial lung disease is long. Yet in some cases, the causes are never found. Disorders without a known cause are grouped under the label of idiopathic interstitial pneumonia, the most common and fatal of these is idiopathic pulmonary fibrosis.
Symptoms of Interstitial Lung Disease
The primary Symptoms of ild disease are
- Shortness of breath at rest and worse with exertion
- Dry cough
Before the appearance of the symptoms, irreversible lung damage has already started. Nevertheless, it is important to consult your doctor about the first signs of respiratory problems. Many conditions other than interstitial lung disease can affect your lungs, and an early and accurate diagnosis is important for proper treatment.
Complications of Interstitial Lung Disease
- Pulmonary hypertension
- Right side heart failure
- Respiratory failure
Types of Interstitial Lung Disease
There are about five broad or main groups of interstitial lung disease
- Occupational related (asbestosis, silicosis, hypersensitivity pneumonitis)
- Treatment-related: chemotherapy, radiation therapy, some medications
- Autoimmune tissue diseases like lupus, scleroderma, poly or dermatomyositis, rheumatoid arthritis-related ild disease
- Sarcoidosis
- Idiopathic ILDs
Few other types of ild disease are
- Sarcoidosis
- Idiopathic pulmonary fibrosis
- Bronchiolitis obliterans
- Histiocytosis X
- Chronic eosinophilic pneumonia
- Collagen vascular disease
- Granulomatous vasculitis
- Goodpasture’s syndrome
- Pulmonary alveolar proteinosis
Apart from this Respiratory bronchiolitis-associated interstitial lung disease (RB-ILD) is a rare, benign inflammatory respiratory disease
End Stage of Interstitial Lung Disease
As the end of life approaches, changes can occur over the course of days … or weeks. Each person’s experience is unique. Some of the symptoms you may experience are listed below. It is important to report any changes in symptoms to your healthcare team. Your pulmonologist or doctor can provide you with more details and you should communicate with them constantly as the end of life approaches.
- Problems of appetite and swallowing.
- Loss of energy, ability, or desire to speak and retire from family and friends
- They usually feel sleepy or sleepy, because they are very inactive and in the end they become unconscious. It is not unusual to stay in bed or a comfortable chair instead of getting up
- Changes in speed or respiratory model. As the body becomes less active, the need for oxygen is reduced. There may be long breaks between the breaths and the belly can move more and down than the chest. There may also be increased chest or respiratory secretions and heavy, wet breathing due to a buildup of mucus that cannot be coughed up. Keep in mind that this may be more distressing for others than for the person concerned. Medications are available that can help dry up the mucus
- Oxygen request if not already in use and support for other medical equipment. This should not interfere with physical contact.
- Changes in skin color and temperature. The skin can become pale, moist, and slightly cooler just before death
- Involuntary shocks – These are normal and don’t mean anyone is upset or uncomfortable
Diagnosis :
It is difficult to identify ild disease. A large number of conditions fall into this broad category. Additionally, the symptoms of a wide variety of medical conditions can mimic interstitial lung disease, and doctors need to rule them out before making a definitive diagnosis. Following tests may be done to determine ILD disease.
- Laboratory Test – a blood test is done to detect proteins, antibodies & markers of autoimmune due to environmental exposure.
- Chest X-Ray
- Imaging Test – CT Scan is the first step in the diagnosis of Ild disease and EcoCardigram is done to evaluate the pressure on the right side of the heart.
- Pulmonary Function Tests
- Lung Tissue Analysis or Lung Biopsy
Treatment of Interstitial Lung Disease
There is no cure for ild disease. Treatment is given to underlying disease and improving your symptoms. The scarring of the lungs that occurs with interstitial lung disease cannot be reversed, and treatment will not always be effective in stopping the eventual progression of the disease. Some treatments can temporarily improve symptoms or slow down the disease progression thus contributing to improving the quality of life. There are no approved therapies for many types of scarring diseases.
- Medications – Corticosteroids, medicines to slow the progression of the disease, and medicine that reduce stomach acids.
- Oxygene Therapy to stop lung damage
- Pulmonary Rehabilitation
- Surgery includes lung transplantation
Conclusion
Since there are many types of interstitial lung disease, each case can be mild or very severe. Most types of ild disease cause irreversible lung damage. The most severe ILDs are progressive, with your condition continuing to worsen over time. Severity and cause determine the life expectancy for ILD disease. Some people with mild PID can lead normal lives with little or no treatment. Your outlook (prognosis) is better if your disease does not get worse. For people with the most severe, rapidly worsening forms of interstitial lung disease, life expectancy is about 3 to 5 years after diagnosis.

 Previous Post
Previous Post Next Post
Next Post